By Bachem AG
Bachem antihypertensive food-derived peptides
Bachem offers a number of readily available synthetic antihypertensive peptides, which have gained considerable interest as nutraceutical ingredients in functional food.
Antihypertensive peptides from food proteins have been identified and studied in vitro and in vivo as potentially having a valuable positive supplementary influence on reducing blood pressure.
A large number of these peptide sequences act by inhibition of angiotensin-converting enzyme (ACE), a key enzyme in blood pressure regulation, which is also the target of many common antihypertensive drugs. However, many antihypertensive peptides mediate their effects by other mechanisms or affect different regulators of blood pressure.
Hypertension types and causes
Hypertension is considered a silent killer as it rarely causes symptoms. According to the WHO, it affects about 1 billion people worldwide and is responsible for the deaths of approximately nine million annually, largely as an established risk factor for the development of cardiovascular diseases (CVD), stroke, and kidney diseases.
- Primary hypertension, or ‘essential hypertension’, has no clear etiology but is the most prevalent type and affects 90-95% of hypertensive patients.
- Secondary hypertension arises from an identifiable cause such as kidney disease or adrenal disease. It can also arise from medication. It is diagnosed in 5-10% of the hypertensive patients. The treatment of secondary hypertension depends on its cause. First line medications to treat essential hypertension include calcium channel blockers, angiotensin-converting enzyme (ACE) inhibitors, angiotensin receptor blockers, and thiazide diuretics.
Behavioral risk factors for hypertension include physical inactivity, poor stress management, harmful levels of alcohol use, high sodium and fat intake and other dietary habits such as not eating enough fruit and vegetables. Genetic factors also contribute to the risk of developing hypertension with patients with family history of hypertension more likely to develop the condition. Metabolic factors that increase the risk of heart disease, stroke, kidney failure and other complications of hypertension include diabetes, high cholesterol and obesity.
Hypertension Mechanisms
The body uses several mechanisms to regulate arterial blood pressure in order to ensure adequate blood flow to all organs in the body.
Baroreceptor Reflex enables the body to respond to acute changes in blood pressure detected by baroreceptors, stretch-sensitive mechanoreceptors within blood vessels that send impulses to the central nervous system and thereby reflexively influence peripheral vascular resistance and cardiac output.
Vasopressin: Also known as an antidiuretic hormone, this nine-amino acid peptide secreted from the posterior pituitary is synthesized in the hypothalamus and transported via the hypothalamic-hypophyseal tracts to the posterior pituitary where it is stored until released upon nervous stimulation. Vasopressin is released in response to triggers such as low blood pressure monitored by high-pressure baroreceptors, and acts on the kidneys to increase blood volume by constriction of the blood vessels.
Renin-Angiotensin-Aldosterone System (RAAS): A major regulator of arterial pressure and plays a key role in the pathogenesis of essential hypertension. Renin is the initiative enzyme that is expressed in the juxtaglomerular cells of the kidney and secreted into the circulation in response to decreased renal blood pressure, decreased salt delivery to the distal convoluted tubules of the nephrons, and/or β-agonism.
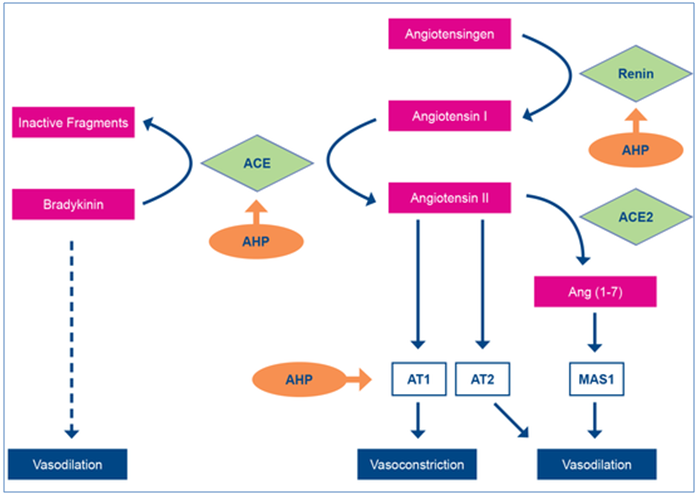
Angiotensin: The product of plasma renin acting on angiotensinogen, cleaving it first into angiotensin I, which is subsequent cleaved by ACE to yield angiotensin II. (Figure 1). Angiotensin II functions in many ways to increase arterial pressure including vasoconstriction of arterioles by binding to AT1 receptors, release of vasopressin from the posterior pituitary and release of aldosterone from the adrenal cortex.
Aldosterone causes the distal convoluted tubules to increase reabsorption of sodium and to increase secretion of potassium. The increase in sodium reabsorption leads to passive reabsorption of water and an increase in blood pressure.
Food-derived Antihypertensive Peptides
Many food-derived proteins contain antihypertensive peptides encrypted in their protein sequences. They can be released during gastrointestinal transit or by food processing such as enzymatic hydrolysis or fermentation.
In many cases, the antihypertensive effect is mediated through inhibition of ACE but antihypertensive peptides can also interact with renin, endothelin-converting enzyme (ACE), angiotensin receptors, calcium channels, and opioid receptors and play a role on the endothelin system function, arginine-nitric oxide pathway, and vascular remodeling.
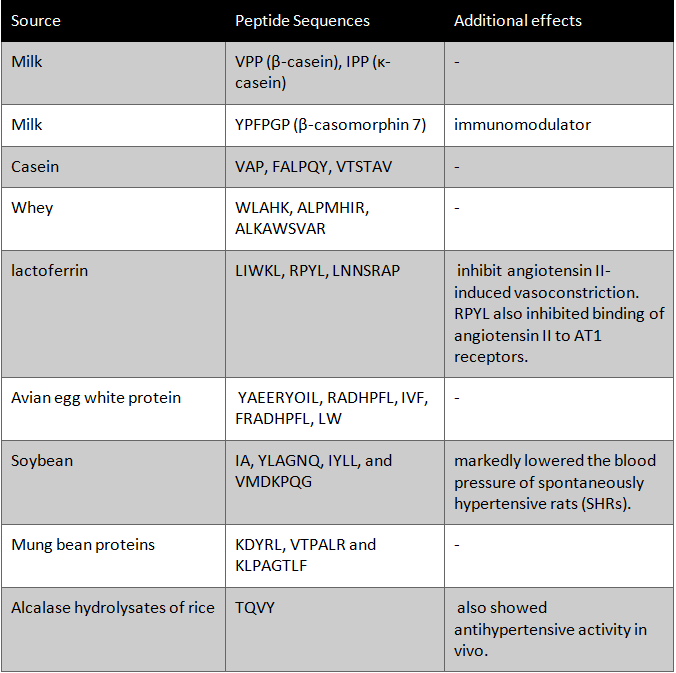
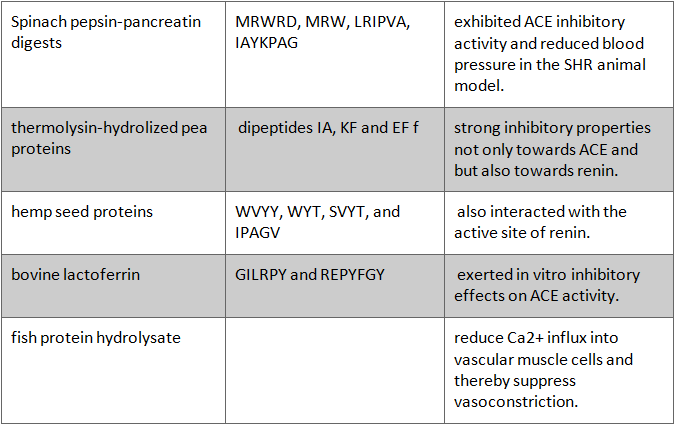
In the literature, numerous ACE inhibitory peptide sequences have been described including sequences isolated from dairy products, egg, meat or fish, as well as plant sources. These various peptide groups and sources are tabulated below:
Bachem Antihypertensive Peptides
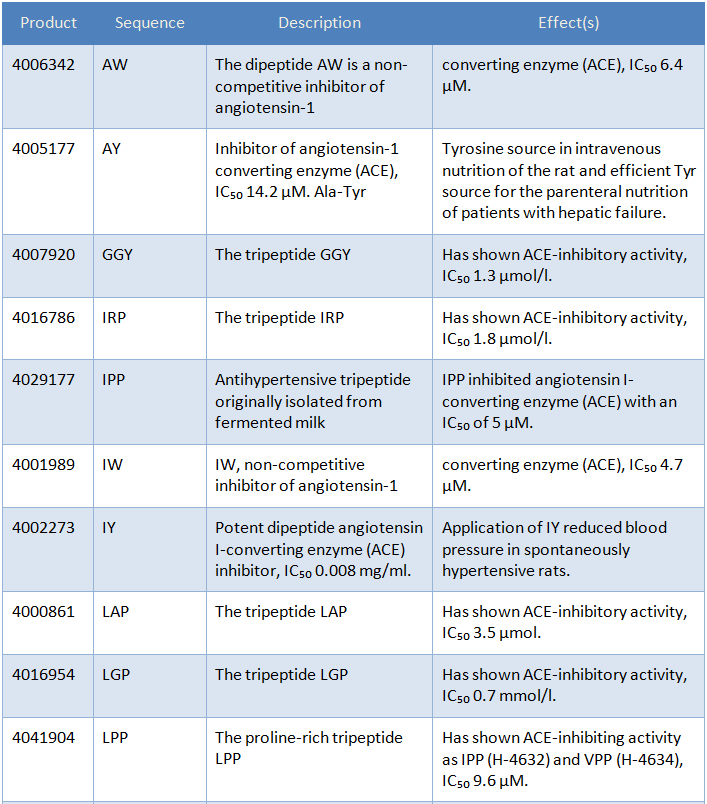
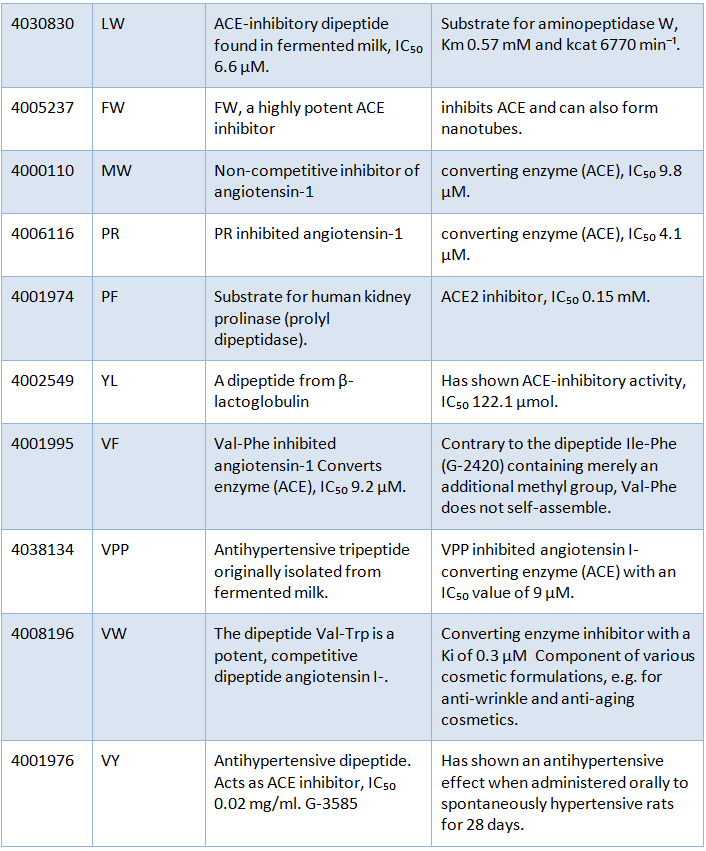
Bachem offers a number of readily available synthetic antihypertensive peptides, tabulated below. It can also support specific research with an excellent custom synthesis service.
There is interest in the use of natural food based products to prevent and treat hypertension. In the future, new clinical studies are anticipated to show how various food-derived peptides can contribute to blood pressure control and provide other health benefits.
However, it should be noted that antihypertensive food-derived peptides so far form a promising adjunct to blood pressure reduction antihypertensive drugs, which remain indispensable.
Resources
Click on Bachem products to browse Bachem online shop.
Click on Bachems News to see latest News & Events.